
News
SARS-CoV-2 can trigger chronic fatigue syndrome
31.08.2022 / SARS-CoV-2 has long been suspected of causing chronic fatigue syndrome (ME/CFS). A team of researchers from Charité and Max Delbrück Center now provides scientific evidence in the journal “Nature Communications”. The researchers also describe a similar clinical picture with a presumably different cause.
“Suspicions that COVID-19 might trigger ME/CFS initially arose as early as during the first wave of the pandemic,” says Prof. Dr. Carmen Scheibenbogen, Acting Director of Charité’s Institute of Medical Immunology on Campus Virchow-Klinikum. Carmen Scheibenbogen also oversees the work of the ‘Charité Fatigue Center’, which specializes in the diagnosis of ME/CFS (myalgic encephalomyelitis/chronic fatigue syndrome), a debilitating condition characterized by severe physical fatigue. The center received its first requests from patients after SARS-CoV-2 infection as early as the summer of 2020. Since then, there has been accumulating evidence of a causal link between COVID-19 and ME/CFS, a disease which often causes severe physical impairments.
“Providing the scientific evidence to confirm these assumptions, however, is anything but a trivial task,” explains Carmen Scheibenbogen. She continues: “This is partly due to the paucity of research into ME/CFS and the fact that there are no universally accepted diagnostic criteria. Thanks to an extremely thorough diagnostic process and a comprehensive comparison with patients who developed ME/CFS following non-COVID-related infections, we have now been able to show that COVID-19 can trigger ME/CFS.”
Even after mild COVID-19
As part of this study, experts from Charité’s Post-COVID Network examined 42 individuals who presented at the Center with persistent, severe fatigue and impaired day-to-day functioning six months after their SARS-CoV-2 infection. Most of the study participants were unable to perform light work for more than two to four hours a day; some were unable to work and struggled to look after themselves. Only three out of the 42 patients examined needed hospital care during their initial (acute) SARS-CoV-2 infection, but none required oxygen. 32 of the patients met the WHO classification of mild COVID-19, meaning they did not develop pneumonia, but had fairly severe symptoms including fever, cough, muscle pain and joint pain for between one and two weeks. As all of the participants’ infections occurred during the first wave of the pandemic, none of them had been vaccinated. At Charité, all of the individuals concerned were examined by an interdisciplinary team of neurologists, immunologists, rheumatologists, cardiologists, endocrinologists and pulmonologists with many years’ experience in the diagnosis of ME/CFS. For comparison, the researchers then examined 19 age- and gender-matched individuals who had developed ME/CFS following a similar period of illness due to a non-COVID-related infection.
Reliable diagnosis
The researchers used the ‘Canadian Consensus Criteria’ to establish a diagnosis of ME/CFS. “In addition to having been scientifically developed, this catalog of criteria has been proven as a reliable diagnostic tool for chronic fatigue syndrome in clinical practice,” explains the study’s other co-lead, Dr. Judith Bellmann-Strobl, who heads the multidisciplinary outpatient department at the Experimental and Clinical Research Center (ECRC), a facility jointly operated by Charité and the Max Delbrück Center.
According to the Canadian Consensus Criteria, approximately half of the post-COVID patients examined met the diagnostic criteria for ME/CFS. While the other half presented with similar symptoms, their post-exertional malaise was milder and only lasted for a few hours. In contrast, ME/CFS patients reported post-exertional malaise which persisted into the following day. Summarizing the researchers’ findings, Dr. Bellman-Strobl says: “We can therefore distinguish between two groups of post-COVID patients with severely impaired physical functioning.”
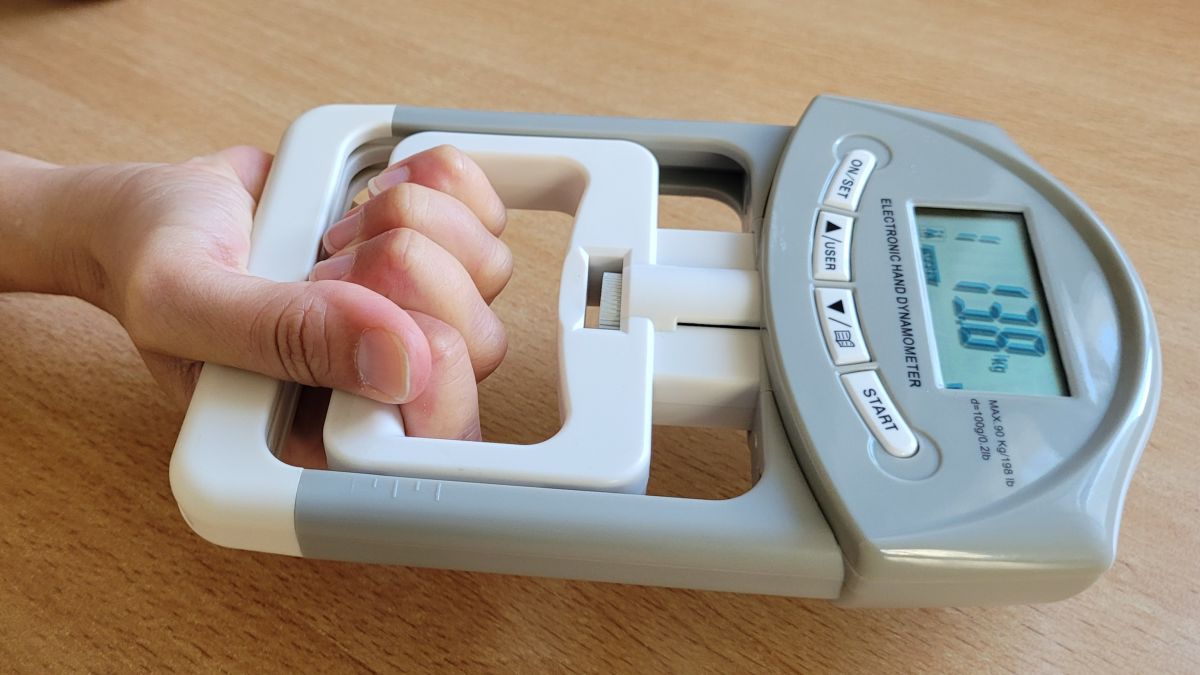
Reduced hand grip strength
In addition to collecting data on symptoms, the researchers also determined various laboratory parameters. They then compared these with hand grip strength, which was reduced in the majority of the participants examined. “We furthermore found that individuals with milder exertional intolerance had reduced hand grip strength if they had elevated levels of the cytokine interleukin 8. In these cases, reduced muscular strength may be caused by a persistent inflammatory response,” says Carmen Scheibenbogen. “In the ME/CFS group, however, hand grip strength was correlated with the hormone NT-proBNP, which can be released by muscle cells when oxygen supply is insufficient.
This suggests that, in these individuals, muscle weakness may be caused by an impaired blood supply.” According to the researchers’ preliminary observations, the two groups may also be distinguishable in terms of disease progression. “In many people whose symptoms are indicative of ME/CFS but who do not meet diagnostic criteria, symptoms appear to improve over time,” explains Carmen Scheibenbogen.
ME/CFS is not psychosomatic
These new findings may help researchers to develop specific treatments for post-COVID syndrome (‘Long Covid’) and ME/CFS. “Our data also provide further evidence that ME/CFS is not a psychosomatic disorder but a severe physical disease which can be measured and diagnosed using objective methods,” emphasizes Carmen Scheibenbogen. “Unfortunately, current treatments for ME/CFS are purely symptomatic in nature. I would therefore urge even young people to protect themselves against SARS-CoV-2 by getting vaccinated and wearing a FFP2 mask.”
Further information
- Charité Fatigue Center
- Neuroimmunology Outpatient Clinic, ECRC
- Charité’s Post-COVID Network
- Institute for Medical Immunology
- Press photos by the German Association for ME/CFS
Literature
Claudia Kedor et al (2022): Post COVID-19 Chronic Fatigue Syndrome following the first pandemic wave in Germany and biomarkers associated with symptom severity results from a prospective observational study, in: Nature Communications, DOI: 10.1038/s41467-022-32507-6
A summary of current scientific knowledge on ME/CFS after COVID-19 can be found in Prof. Scheibenbogen’s recent review article (German only):
Herbert Renz-Polster, Carmen Scheibenbogen (2022): Post-COVID-Syndrom mit Fatigue und Belastungsintoleranz: Myalgische Enzephalomyelitis bzw. Chronisches Fatigue-Syndrom, in: Die Innere Medizin, DOI: 10.1007/s00108-022-01369-x
Download
Source: Joint press release of Max Delbrück Center and Charité - Universitätsmedizin BerlinSARS-CoV-2 can trigger chronic fatigue syndrome